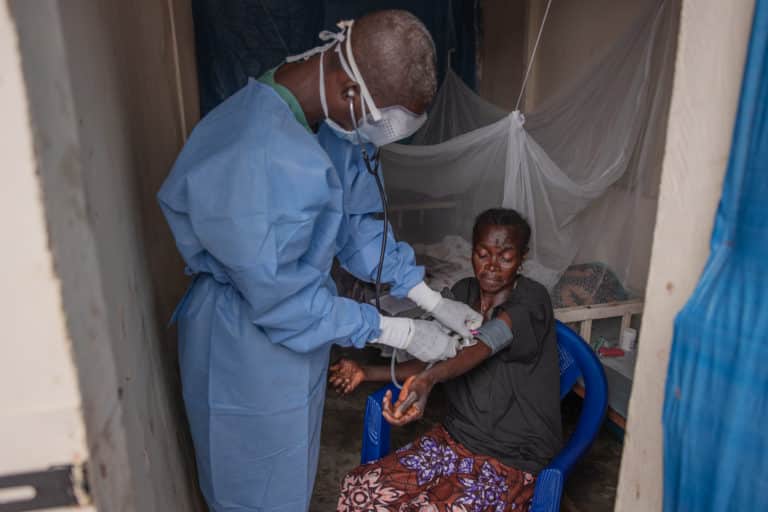
If you talk with any of the patients, healthcare workers or other hospital staff, you will discover a common thread among the discussions: fear. Fear of being contaminated, fear of infecting someone else, fear of suffering, fear of dying, fear of being stigmatized.
“At the beginning, I was stressed about the idea of working in the department that is closest to the patients infected [with COVID-19],” recalls Jeanne Kontchiachou Atyame, a secretary working in the Isolation Unit at the Yaoundé Central Hospital.“I was afraid for my own health.”
Here, as elsewhere, “many people still take the pandemic lightly” Jeanne laments. As of August 10th, there were 17,586 confirmed cases and 393 deaths in Cameroon.
In the triage area set up in March by ALIMA, in partnership with the Cameroonian Ministry of Health, patients are worried.
Pauline Diane Mahouve Djeni, is among a group of patients seated under the white tarpaulin tent. The 30-year-old came voluntarily, with her husband, after having been in contact with a person who tested positive for COVID-19.
“I am very anxious” she admits, waiting to receive the results of her COVID-19 test. “If the result is positive, I’m afraid of infecting my children. And then everyone I’ve been in contact with is going to have to be tested.”
Jeanne and Pauline are not the only ones. Maxence Momha Ngo, an emergency physician with the Ministry of Health at the hospital, says she sees this every day.
“How do you respond when a patient tells you that he or she is afraid of isolation?” she asks. “As a doctor, I don’t have an answer to that question.”
Within the triage unit, ALIMA quickly put in place a psychological support system.
In front of the isolation zone, emergency doctor Maxence Ngo Momha, 28, and some members of the
NGO ALIMA discuss the situation. Yaoundé, Cameroon, July 2020. © Daniel Beloumou / ALIMA
“The unprecedented nature of this global health crisis is very worrying for people,” explains Valérie Chanfreau, ALIMA’s mental health advisor. “People respond to it differently: some by obsessively cleaning, some by denying the illness, and in other ways. These are very powerful mechanisms that influence a person’s physical health,” emphasizes the clinical psychologist. “For good care, you have to look at the person as a whole.”
Since 1993, the World Health Organization has been recommending that psychosocial care (mental health and psychosocial support) be integrated into all public health responses. In Cameroon, comprehensive patient care, both physical and psychological, is not yet very developed. Additionally, there is a glaring lack of psychologists.
To help improve psycho-social support, ALIMA has been integrating psychological components within its humanitarian medical emergency programs since 2014. At the Yaoundé Central Hospital, the team offers health professionals training modules on stress management for response teams, patients and their families. The aim: to help them understand the psychological mechanisms linked to mental illness and to strengthen the quality of the health worker-patient relationship.
Portrait of psychologist Taïki Foka Simon, within the triage area of the Central Hospital in Yaounde, Cameroon. © Daniel Beloumou / ALIMA
Simon Taïki Foka is part of the team that must ease the fears of both patients and hospital staff.
“My job is to support people, to guide them: I’m here to help,” says the clinical psychologist. Every day, along with the team in the triage unit, he counsels people, explaining how the test is going to be done and preparing people to receive their results. His mission: to prevent the positive result of a COVID-19 test from having a negative impact on morale, and creating a sense of overwhelming anxiety or sadness.
“Moving from a healthy person to a sick person is a change of status that is difficult to accept,” explains Valérie Chanfreau. Simon also accompanies the medical team when the results are announced. Individually, he welcomes and listens to each patient to assess their psychological state, and can also meet the families, as the relationship is sometimes difficult.
The nursing staff also require special attention.
“Despite prevention and protective measures, there are people who find themselves in situations where they can be contaminated,” says Valérie Chanfreau. In Africa, as of August 5, 2020, 15,662 health workers have been contaminated. And this fear of disease can be reflected in patient care – which is why Simon brings staff together regularly for discussion groups and workshops on relaxation through music.
—————————-
*Cover photo: © Daniel Beloumou / ALIMA
The ALIMA project to respond to COVID-19 in Cameroon receives financial support from the French Development Agency (AFD).